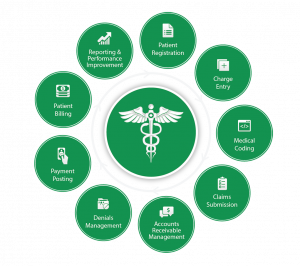
10 Key steps in the Medical Billing Process
What is Medical Billing?
Medical Billing is basically a payment practice or process for a healthcare system of getting a medical facility or physician paid for their services. More or less the same practice is followed in each country for the medical services provided to patients. But here we will discuss the medical billing process within the United States healthcare system and the 10 key steps in the medical billing process.
Patient Check-in:
The medical billing process starts with a patient visit to an Emergency Center, Physician Clinic, Urgent care Center, Hospital, or any other medical facility. A patient can visit or check in at any Physician Clinic by walk-in or through a scheduled appointment, but Emergency Center, Hospital, and Urgent care patients can visit or check in on an urgent basis.
Patient Registration:
When a patient arrives at a physician’s clinic, urgent care, emergency center, or a hospital, the next step is patient registration. Administration staff at the front desk will provide a registration form to the patient or they will take the information to enter into the registration system. The patient registration form includes information about the patient, Insurance information, billing address, contact information, etc. After the administration staff has the registration information, the physician evaluates the patient.
Charting or Medical Documentation:
During the patient’s evaluation process or treatment, physician or nurse documents all the procedures, treatments, diagnoses, prescriptions, etc in paper format or in EHR (Electronic Health Records). It is also called, Medical Charts, Medical records, Medical Notes, and Clinical information, etc.
Medical Coding:
Once medical documentation or charting is completed by a physician, a specialist coder take this information to assign appropriate Procedures Codes/CPT’s and Diagnosis/ICD-10 for the billing team.
Medical Billing:
Medical billers enter these procedures/CPT’s, Diagnosis/ICD-10, and Date of Service into Billing Software or review them if already entered by the Coders and get the claims ready for Insurance Submission.
Claims Submission:
Once claims are ready from the billing team, they are sent to the Insurance either as paper mail out or through electronic submission via a clearing house (EDI 837). If the claim is being submitted electronically, the claim will be filtered by a Clearing House to make sure that a clean claim is being submitted to the Insurance without any error.
Follow-up with Insurance:
Once the claims are submitted to the Insurance, Insurance will review the claims, and the physician or medical facility will be paid by the Insurance company. If payment isn’t received in a standard time frame then the Follow-up team will follow-up with the Insurance company to inquire if the claim is paid, or denied. If a claim is denied due to any reason or missing information, the Follow-up team will further work on the claim to get it paid.
Payment from Insurance:
Explanation of the paid claim is either sent in an electronic format “ERA” (EDI 835) or in a paper format “EOB” that is mailed out on the physician’s or medical facility’s address. Payments are made either directly into the bank (ACH, EFT) or a check is issued along with the “EOB” in the physician’s or medical facility’s name which can be deposited into the bank.
Payment Posting:
Once the billing team has received the ERA (ERA in the Billing Software) or EOB (EOB from the physician’s or medical facility), they will post the payment information into the Billing Software against the claim that was sent to the Insurance.
Patient Statement:
Once the payment is posted into the Billing Software, the last step is to send the patient statements for any patient responsibility left by the Insurance company in terms of Coinsurance, Copay, or Deductible. Patient statements are mailed out on the patient’s mailing address and the patient sends the payments to the physician or pay it online. Normally, Copay is paid by the patients upfront at the time of the visit.
Interested in Learning RCMXpertz‘s Medical Billing & Revenue Cycle Management Process?